Facility Details
View an overview of the medical facility, affiliated physicians, and available programs in one place.
- 治療
- 整形外科
- 整形外科
- 脊椎
- 関節症
Independent Administrative Institution National Hospital Organization Murayama Medical Center
The hospital specialized in spine-spinal cord surgery with 14spine surgeons. Special emphasis is placed on minimallly invasive surgeries such as skip laminoplasty, and CBT methods. We provide patient-friendly surgeries that minimize muscle damage and post-operative pain.
Our hospital specializes in spine and spinal cord surgery, with 14 spine surgeons dedicated to this field.
Among our 33 full-time physicians, 20 are orthopedic surgeons, including 14 spine specialists.
In addition to providing a wide range of general orthopedic surgeries, we place particular emphasis on minimally invasive spinal surgery.
For cervical spine decompression, we perform skip laminoplasty, and for lumbar spinal fixation, we use the Cortical Bone Trajectory (CBT) technique.
These surgical techniques minimize muscle damage as much as possible, reduce postoperative pain, and provide patient-friendly surgical treatment.
Our hospital is equipped with advanced medical technology, including four surgical microscopes and a navigation system, enabling highly precise and safe procedures.
For more information, please visit:
https://www.instagram.com/murayamamedical/?utm_source=qr
- Location
- 〒208-0011
2-37-1 Gakuen, Musashimuurayama-shi
- Website
- https://murayama.hosp.go.jp
- Facility Overview
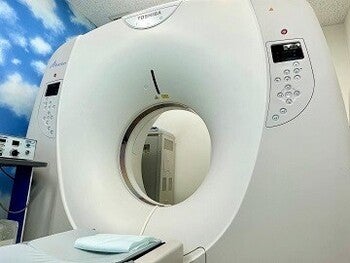
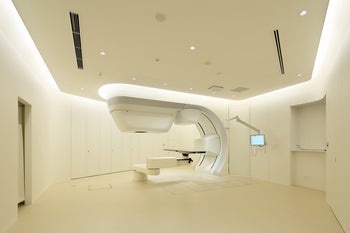
- 【Location】It is located in a quiet environment in the suburbs of Tokyo. It is a large site with a lot of greenery and a tranquil atmosphere. 【Equipped medical devices】MRI, CT, intraoperative electric stimulator, surgical microscope, intraoperative navigation system , rehabilitation for quadriplegic patients.
【Equipment in facility】MRI, CT, intraoperative electric stimulator, surgical microscope, intraoperative navigation system , rehabilitation for quadriplegic patients.
【Others】Since the 1960s, our hospital has maintained its tradition as a hospital specializing in spinal cord care while also incorporating state-of-the-art medical care. The ward was constructed in 2019 and has spacious corridors and a calm environment. The number of spinal cord surgeries is one of the highest in Japan, with 1,200 per year.
- Specialty
- Spinal cord surgery Artificial hip joint surgery Artificial knee joint surgery
Available Programs
-
skip laminoplasty(Murayama Medical Center)
This procedure is a muscle-preserving minimally invasive posterior cervical decompression surgery.
A surgical microscope is used to minimize the size of the incision and the extent of the surgical field, allowing decompression to be performed only at the affected area.
Although this technique requires a very high level of surgical expertise, it involves minimal bleeding and mild postoperative pain, providing a patient-friendly surgical treatment.
This surgery is indicated for conditions in which nerves in the cervical spine are compressed, leading to symptoms such as numbness, pain, or paralysis.
Typical conditions include:
Cervical disc herniation
Cervical spondylosis
Ossification of the posterior longitudinal ligament (OPLL)This procedure is a muscle-preserving minimally invasive posterior cervical decompression surgery. Using a surgical microscope, the incision range and surgical field are minimized, and only the affected area is decompressed. Although this surgery requires highly advanced surgical techniques, it involves minimal bleeding and reduced postoperative pain, providing a patient-friendly surgical treatment. This procedure is indicated for conditions in which nerves in the cervical spine are compressed, causing symptoms such as numbness, pain, or paralysis. Typical conditions include: Cervical disc herniation Cervical spondylosis Ossification of the posterior longitudinal ligament (OPLL) Depending on the extent of the lesion, the surgery is performed under general anesthesia with a 4–8 cm vertical incision on the back of the neck. The muscles attached to the bone are preserved as much as possible, and only the necessary area is exposed. Using a surgical microscope, the bone is carefully shaved to relieve compression on the spinal cord. Surgery time: approximately 1–2 hours Postoperative care: patients remain in bed for the first 2 days Walking: possible from the 3rd postoperative day Discharge: usually around 10 days after surgery once the wound has stabilized Over the past three years, the hospital has performed an average of 135 surgeries per year. In cervical spine surgery, complete disappearance of symptoms cannot always be guaranteed. Some patients may continue to experience numbness, pain, or residual paralysis. In rare cases, neurological symptoms may worsen. A small number of patients may develop postoperative infections. If this occurs, additional surgery under general anesthesia may be required, resulting in a longer hospital stay. In 2025, the postoperative infection rate was 2.3%.
View Details -
CBTmethod(cortical bone trajectory)(Murayama Medical Center)
This is a muscle-friendly posterior lumbar fusion technique. Using intraoperative fluoroscopy, screws are inserted into the cortical bone (the hard part of the bone) from the inside to the outside and from the caudal to the head. Although technically very advanced, it provides a patient-friendly procedure with minimal blood loss and mild postoperative pain.
This is for conditions where there is instability of the lumbar spine and numbness, pain, and paralysis have appeared. Lumbar disc herniation, lumbar spinal canal stenosis with instability, and lumbar spondylolisthesis are the targets.This procedure is a muscle-preserving posterior lumbar fusion surgery. During surgery, intraoperative fluoroscopy (X-ray imaging) is used to insert screws into the cortical bone (the dense outer layer of bone). The screws are inserted from the medial to the lateral side and from the caudal to the cranial direction. Although this procedure requires highly advanced surgical techniques, it involves minimal bleeding and mild postoperative pain, providing a patient-friendly surgical treatment. This surgery is indicated for patients with lumbar spinal instability causing symptoms such as numbness, pain, or paralysis. Typical conditions include: Lumbar disc herniation Lumbar spinal canal stenosis with instability Lumbar spondylolisthesis Depending on the extent of the lesion, the surgery is performed under general anesthesia with a 5–8 cm vertical incision in the lower back. The muscles are carefully separated to expose the surgical field. Using intraoperative fluoroscopy, screws are inserted into the cortical bone. Compared with conventional techniques, this method requires less muscle detachment and preserves the facet joints, helping to prevent postoperative spinal deformity and reduce bleeding. Surgery time: approximately 2 hours Estimated blood loss: about 50 ml Postoperative care: patients remain in bed for the first 2 days Walking: possible from the 3rd postoperative day Discharge: usually about 10 days after surgery once the wound has stabilized Over the past three years, the hospital has performed an average of 209 lumbar fusion surgeries per year. In lumbar spine surgery, complete disappearance of symptoms cannot always be guaranteed. Some patients may continue to experience numbness, pain, or residual paralysis. In rare cases, neurological symptoms may worsen. A small number of patients may develop postoperative infections. If this occurs, additional surgery under general anesthesia may be required, which may extend the hospital stay. In 2025, the postoperative infection rate was 0.9%.
View Details -
Unilateral invasion bilateral decompression(Murayama Medical Center)
This is a muscle-friendly posterior lumbar decompression. Using an operating microscope, the surgeon decompresses only the lesion while preserving the muscles, joints, and spinous processes on one side. Although technically very advanced, it provides a patient-friendly procedure with minimal blood loss and mild postoperative pain. It is intended for conditions where numbness, pain, and paralysis appear as a result of nerve compression in the lumbar spine. Lumbar disc herniation and lumbar spinal canal stenosis are the targets.
This is a muscle-friendly posterior lumbar decompression. Using an operating microscope, the surgeon decompresses only the lesion while preserving the muscles, joints, and spinous processes on one side. Although technically very advanced, it provides a patient-friendly procedure with minimal blood loss and mild postoperative pain. It is intended for conditions where numbness, pain, and paralysis appear as a result of nerve compression in the lumbar spine. Lumbar disc herniation and lumbar spinal canal stenosis are the targets. Depending on the extent of the lesion, a 4 to 8 cm longitudinal incision is made behind the lumbar region under general anesthesia, and the muscle on one side of the spinous process (bone in the middle of the back) is debrided and expanded. Using a surgical microscope, the vertebral arch (bone behind the lumbar spine) from one side to the contralateral side is shaved and nerve compression is circumferentially decompressed. This completely preserves the continuity of the median lumbar spine and contralateral muscles, and prevents postoperative deformity of the lumbar spine. The surgery takes one to two hours, with a bleeding rate of about 10 ml. Patients are kept in bed for the first two days after surgery, and can walk from the third day. Patients are discharged from the hospital after the wound settles at 10 days postoperatively. The average number of surgeries performed during the last three years was 314 per year. Lumbar spine surgery cannot completely eliminate symptoms. Numbness, pain, and other paralysis can remain. Although rare, it is possible for paralysis to worsen. Postoperative infection occurs in a few patients. In those cases, as reoperation under general anesthesia is required, hospital stay is prolonged. In 2025, the rate of infection was 2.6%.
View Details