Program Details
Information about medical programs provided by each healthcare institution, including treatment details, schedules, etc.,
- Surgery
- ophthalmology
- Surgery
Multidisciplinary Treatment for Breast Cancer 【Kishiwada Tokushukai Hospital】
Enhancing Quality of Life (QOL) for Breast Cancer Patients with a Wide Range of Treatment Options
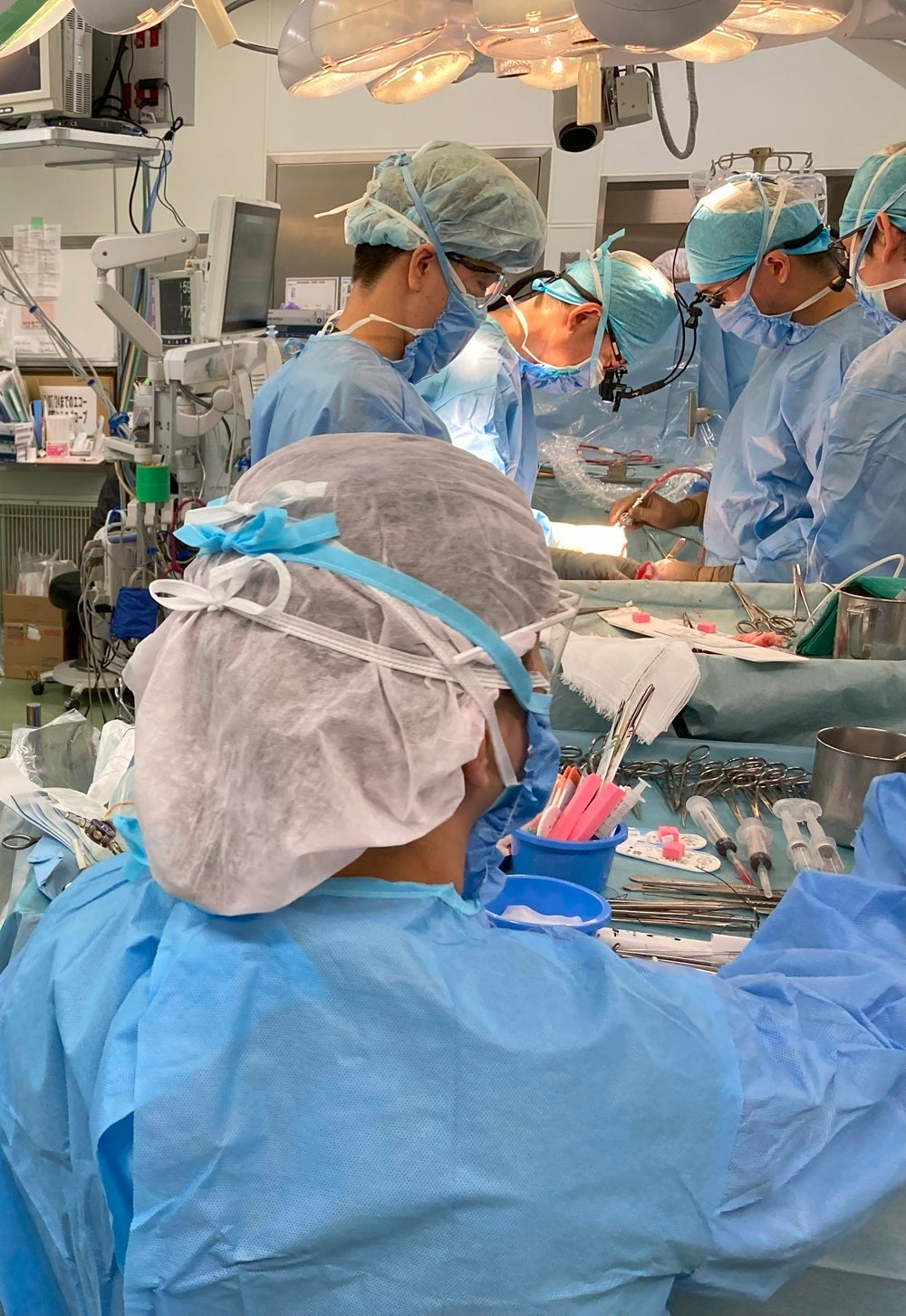
We provide a wide range of treatments, including breast-conserving surgery, reconstructive surgery, chemotherapy, and radiation therapy, aiming to enhance the quality of life (QOL) for breast cancer patients through specialized care.
- Providing Medical Institution
-
Kishiwada Tokushukai Hospital
〒596-0042https://kishiwada.tokushukai.or.jp/en/
4-27-1 Kamoricho, Kishiwada City- Specialty
- **Cardiovascular Surgery:**
1. Coronary Artery Disease
2. Heart Valve Disease
3. Aortic Aneurysm
4. Aortic Dissection
5. Arteriosclerosis Obliterans
6. Arterial Thrombosis
7. Complications of Myocardial Infarction
- Ischemic Cardiomyopathy
- Left Ventricular Rupture
- Left Ventricular Aneurysm
- Ventricular Septal Rupture
- Papillary Muscle Dysfunction (Mitral Regurgitation)
8. Infective Endocarditis
9. Intracardiac Tumors
**Cardiology:**
1. Ischemic Heart Disease (e.g., Angina, Myocardial Infarction)
2. Lower Limb Arteriosclerosis Obliterans
3. Arrhythmia
4. Heart Valve Disease
5. Aortic Stenosis
6. Mitral Regurgitation
**Lower Gastrointestinal Surgery**
*Da Vinci Si - Robot-Assisted Surgery*
1. Malignant Diseases
2. Surgical Treatment of Small and Large Intestine Diseases
3. Primarily Surgical and Medical Treatments for Colon and Rectal Cancer
4. Robot-Assisted Surgery
5. Laparoscopic Surgery
6. Multimodal Therapy Combining Surgery, Chemotherapy, and Radiation Therapy
7. Systemic Chemotherapy for Unresectable Colorectal Cancer
**Breast Surgery:**
1. Breast-Conserving Surgery
2. Mastectomy
3. Sentinel Lymph Node Biopsy
4. Lymph Node Dissection
5. Breast Reconstruction Using Autologous Tissue
**Neurosurgery:**
1. Stroke
2. Cerebral Hemorrhage
3. Subarachnoid Hemorrhage
4. Cerebral Infarction
5. Head Trauma
6. Traumatic Intracranial Hematoma
7. Skull Fracture
8. Chronic Subdural Hematoma
9. Brain and Spinal Cord Tumors
10. Acoustic Neuroma
11. Pituitary Tumor
12. Meningioma
13. Metastatic Brain Tumors
14. Functional Neurological Disorders
15. Facial Spasm
16. Trigeminal Neuralgia
17. Epilepsy
18. Normal Pressure Hydrocephalus
**Urology**
*Da Vinci Si - Robot-Assisted Surgery*
1. Robot-Assisted Laparoscopic Radical Prostatectomy
2. Prostate Cancer
3. Renal Cancer
4. Upper Urinary Tract Cancer
5. Urolithiasis (Urinary Stones)
**Radiology:**
1. Comprehensive Imaging Diagnosis (X-ray, Ultrasound, CT, MRI, Angiography, PET)
2. Liver Tumors
3. Gastrointestinal Hemorrhage
4. Arterial Embolization for Hemoptysis and Traumatic Hemorrhage
5. Transcatheter Venous Embolization for Gastric Varices
6. Intra-Arterial Chemotherapy for Cancer
7. Reservoir Placement
8. CT-Guided Biopsy (Interventional Radiology - IVR)
9. TomoTherapy - Radixact
**Dialysis**
*Travel Hemodialysis* (Available for Individual Travelers Only, Not for Groups)
**Other**
*Second Opinion* (In-person Only, Online Not Available)
- Eligibility Criteria/Exclusions for Treatment
- Eligibility Criteria
1. Medical Information:
- Diagnosis (e.g., breast cancer, breast cancer with bone metastasis)
- Stage and progression of cancer, tumor location (e.g., feasibility of nipple preservation)
- Examination results from other institutions (e.g., mammogram, MRI, CT, PET)
- Presence of comorbidities (e.g., diabetes, heart disease, kidney disease)
2. History of Treatment:
- Previous breast cancer treatment history (e.g., surgery, chemotherapy, radiation therapy)
- Current medications (e.g., anti-cancer drugs, anticoagulants, hormone therapy)
- Allergies or adverse drug reactions
3. Physical Fitness and Age:
- Assessment of whether elderly patients or those with underlying conditions can tolerate surgery, chemotherapy, or radiation therapy
- Evaluation of suitability for reconstructive surgery or drug therapy
4. Preoperative Testing and Preparation:
- Ability to undergo required preoperative tests (e.g., blood tests, ECG, tumor marker tests)
- Capability to manage preoperative lifestyle adjustments and maintain health during drug therapy
5. Postoperative Follow-Up and Lifestyle Guidance:
- Ability and willingness to participate in regular follow-up visits and postoperative care
- Adherence to lifestyle guidance and side effect management during radiation or chemotherapy
- Precautions / Contraindications
- Precautions and Contraindications
1. Cases Not Suitable for Treatment:
- Treatment may be restricted for patients with severe heart or kidney disease who cannot tolerate surgery or chemotherapy.
- Patients unable to receive radiation therapy (due to conditions such as dermatitis or radiation hypersensitivity) or those with allergic reactions to anticancer drugs or hormone therapies may require alternative treatment approaches.
- In cases where cancer has widely metastasized, surgery may not aim for a cure but focus on symptom relief.
2. Postoperative and Treatment-Related Side Effect Risks:
- Postoperative risks such as infection, blood clots, and lymphedema require diligent wound care and effective blood flow management.
- Chemotherapy and radiation therapy may cause nausea, hair loss, fatigue, and immune suppression, requiring regular management of side effects.
- Bone metastasis treatments may increase the risk of fractures, requiring guidance to reduce physical strain in daily activities.
---
# Important Pre-Treatment Information
1. Preoperative Preparation:
- Patients taking anticoagulants or antiplatelet drugs may need to discontinue them before surgery under medical supervision.
- Preoperative tests (e.g., blood tests, CT, ECG) are necessary to confirm surgical eligibility and overall health.
2. Side Effect Management and Follow-Up:
- During chemotherapy or radiation therapy, side effects such as nausea, numbness, and fatigue may occur and should be managed in consultation with a physician.
- Monitoring physical changes during and after treatment is crucial, and any abnormalities should be promptly reported to a healthcare provider.
3. Lifestyle and Daily Precautions:
- Since immune suppression is common, infection prevention (e.g., hand hygiene, avoiding crowded places) is essential, along with maintaining a balanced diet and adequate rest.
- Rehabilitation guidance should be followed to gradually restore daily routines while being mindful of physical limitations.
4. Regular Follow-Up:
- Post-treatment, regular outpatient visits and tests are necessary to monitor progress and detect signs of recurrence or metastasis.
- Early consultation with a physician is critical if symptoms recur or health conditions change.
5. Emergency Response:
- Contact a medical institution immediately in case of fever, severe pain, bleeding, or infection after surgery or during treatment.
- Ensure that emergency contact information for medical institutions and attending physicians is readily available.